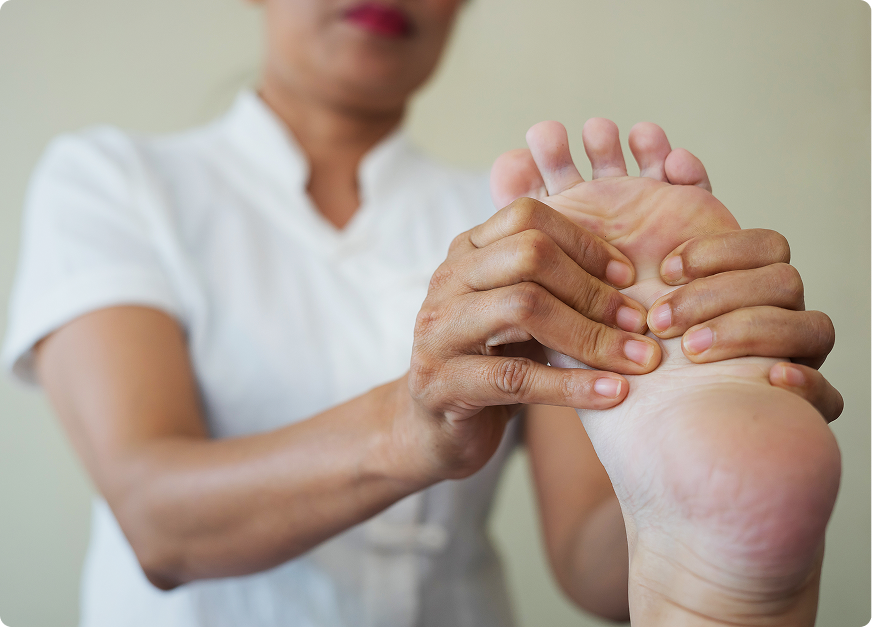

Diabetic wounds develop differently from typical injuries. High blood sugar levels damage blood vessels and nerves over time, creating conditions where even minor cuts, scrapes, or blisters can escalate into chronic, non-healing ulcers if not promptly addressed.
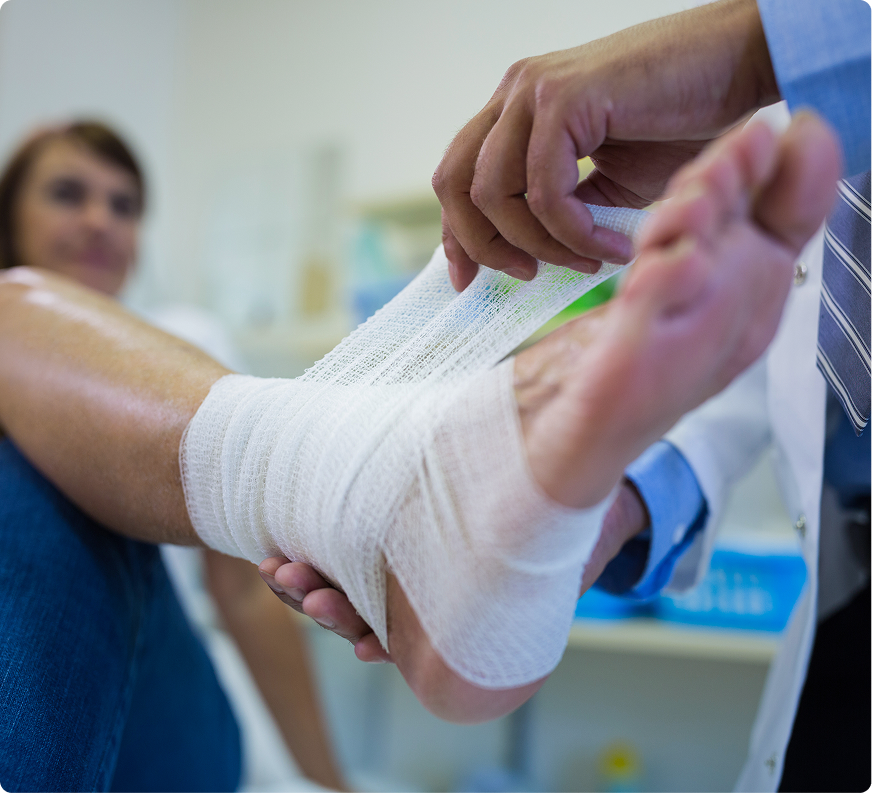
Diabetic foot ulcers (DFUs) are open sores or lesions that typically develop on pressure points of the foot, such as:

Our diagnostic process includes:
Detailed visual inspection of the wound
Assessment of size, depth, and characteristics
Evaluation of surrounding skin integrity
Documentation using standardized protocols
Complete medical history focusing on diabetes management
Tracking healing progress objectively





The cost of diabetic wound care in Novi, Southfield, Howell, and Livonia, MI, can vary significantly depending on wound complexity and treatments required. Patients can expect a range of $150 to $800 per visit, excluding specialized procedures, such as HBOT.
This range is an estimate, and actual costs depend on:
We recommend contacting our office for a personalized quote based on your specific needs.